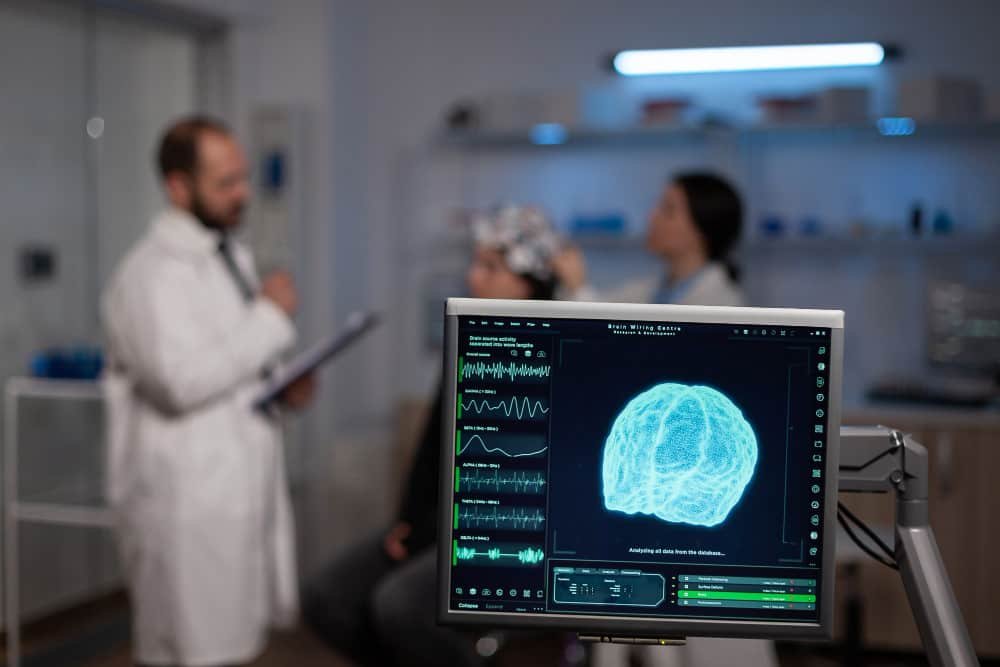
Whenever we talk about brain tumor surgery, the patient and the relatives get frightened and become very uncomfortable, as for them it is a life threatening condition. But with time the brain tumor surgery has evolved significantly and the outcome is quiet promising.
The person who do it is a neurosurgeon. He is a very skillful person in managing such conditions. There is a whole team of people working with him day and night, to manage the patient pre-operative, operative and post-operative period. Sometimes, in doing pituitary surgery he needs help of the ENT surgeon as he creates the pathway for him from the nose, endoscopically to reach the tumor.
Surgery is the main form of treatment for brain tumor patients. The goal of the surgery is:
- To remove the tumor completely and cure the patient
- To remove the tumor partially so relieve the symptoms, as total excision will result in development of deficit, compromising the quality of life of the patient post operatively.
- If there is any obstruction in the pathway of the cerebrospinal fluid, then drain it, to relieve the obstruction by putting a shunt or endoscopic third ventriculostomy (ETV).
- For putting chemotherapy on the local tumor area, to lower the rate of recurrence.
- And sometimes to take the biopsy of the tumor.
Preparing for a brain tumor surgery:
In order to indentify the exact location of tumor and to plan the procedure, a neurosurgeon will order the following imaging studies:
- MRI which might include the functional MRI and diffusion tensor imaging (DTI).
- CT Scan
- CT Angiogram
Sometimes the fudicial marker (stickers) are used to target a specific area for surgical resection during a CT or a MRI. These create a 3D map of our head when these images are integrated with the neuro-navigation system. Almost similar to a GPS. This helps in precisely locating the tumor and achieve maximum resection without injuring the key areas of the brain.
Surgery of brain tumors are done by two methods:
- Craniotomy
- Neuroendoscopic
Craniotomy:
This is the most common type of operation done for brain tumor patients. In this procedure, firstly we give general anesthesia to the patient, so that he goes into a prolonged sleep and won’t be aware of what is happening in the operation theatre. Then the surgeon gives an incision over the region where the tumor is located. Once the scalp is retracted we reach the skull bone. Then a burr hole is made and craniotomy is done, in which we remove a part of the bone, so that we can enter into brain and do the surgery. While doing this procedure the surgeon uses an operative microscope to have a clearer microscopic view and to differentiate between a normal and tumor tissue. Sometimes, when the tumor is very tough we use a CUSA (cavitron ultrasonic aspirator) so that the tumor is removed easily without putting unnecessary stretch over the surrounding vital structures. After removing the tumor, the bone flap is kept back and fixed using metallic miniplates and screws and scalp is closed.
- Giving a scalp incision to reach the skull
- Doing a Burr hole and separating the dura through the burr hole and cutting the bone to elevate the bone flap.
- Cutting the dura to reach the
- concerned area of the brain.
Awake Craniotomy:
This type of surgery is not very common. It is done mainly in those patients who have a tumor at eloquent areas of the brain which are concerned with very important functions like speech and movements. In this the patient is given a cranial block which blocks the pain sensation and is awake throughout the procedure. During the surgery the patient is given a task while the surgeon is operating like moving the hand or leg or talking. This is done because while operating if the surgeon enters into the concerned area, then that very moment the surgeon get to know and he stops and hence the deficit is prevented with maximum safe resection of the tumor. Some surgeons use electrophysiological monitoring for operating such patients. Once the tumor is removed, bone flap is replaced, fixed and scalp is closed. Throughout the procedure the surgical team makes sure that the patient is comfortable.
Patient is awake while doing the surgery.
Neuroendoscopy:
In this we usually operate tumors which are inside or around the ventricular system (fluid filled cavity) of the brain. In this a small burr hole is made on the skull and through that the endoscope is introduced in the ventricular system. It is used for taking the biopsy and at times complete evacuation of tumor. It is also used in CSF diversion in case of hydrocephalus.
Neuroendoscope is a long tubular instrument which is connected to a light source and camera. The image is seen on the monitor and this is how the surgery is done seeing on the screen. Long slender, thin highly specialized scissors, forceps, bipolar is used to remove the tumor.
Neuro-endoscope with multiple channels to introduce scissors and forceps
Fig. Endoscope introduced inside the ventricles
Fig. Endoscope introduced into the supracerebellar infratentorial to remove the pineal tumor
Pituitary Tumor Surgery:
Pituitary gland is a gland which is located in a cavity called the sella tursica lying at the posterio superior aspect of the nose. So, reaching there is quiet simple through the hollow nose rather than doing a craniotomy. This procedure of operating such tumors is called as a trans-nasal trans-sphenoidal surgery. While doing such procedures the neurosurgeon always takes a help of an ENT and skull base surgeon.
In this procedure the endoscope is introduced through the nose and a small hole is made at the superior aspect of nasal septum, so that both the nostrils reach a common place and from there the instruments can be passed to do the surgery.
Fig. Endoscope introduced through the nose Transnasal Trans-sphenoidal Approach to reach the pituitary tumors
Fig. Endoscopic Exicision of Pituitary Tumor
Surgery for Hydrocephalus:
Inside our brain are the ventricles which are fluid filled cavities inside the brain and in them, there is a continuous formation of cerebrospinal fluid and it circulates through the ventricles to the cerebral convexities and is absorbed through the venous channels. Any obstruction in this flow results in accumulation of fluid in the ventricles called as hydrocephalus. In this condition, we bypass the fluid by putting a shunt or we make a new pathway by creating a hole at the floor of third ventricle called endoscopic third ventriculostomy (ETV).
Fig. Ventriculo-peritoneal Shunt
Fig a) Neuroendoscope introduced into the lateral ventricles
b) Going through the Foramen of munro to reach the third ventricles
c) Floor of third ventricle, endoscopic view
d) After making the puncture a fogarty catheter introduced and balloon is inflated to widen the opening
e) A wide opening made at the floor of the third ventricle.
Surgery for giving Chemotherapy:
There are some tumors like high grade gliomas in which keeping the chemotherapy wafers (implants) locally at the tumor site improves the survival. Sometimes, an Omaya chamber is implanted, which is a ventricular access device to give chemotherapy directly into the ventricles.
Post-operative period:
After the brain surgery is done, the patient is shifted to an intensive care unit, and is put on intra venous fluids and injectables. Post six hours and depending on the neurological status patient can be started on oral diet. The next day morning a follow up scan is done to see for the brain condition inside and the amount of tumor removal achieved. If everything is fine, then the patient is discharged from the hospital in 4-5 days.